Restore movement and reclaim your lifestyle.
Hip arthroplasty
A hip arthroplasty is the removal of the damaged parts of the hip joint, which are then replaced with artificial joints, made from either metal, ceramic or plastic.
It is an extreme surgery that is only performed on people with severe hip damage or osteoarthritis (a degenerative joint disease or degenerative arthritis). It is a viable option for people who have tried more conservative treatment plans, such as physical therapy, pain control and exercise, and are still left in pain and with hindered mobility.
A hip replacement can help to relieve pain, assist the hip joint to function better and improve mobility.
THE HIP
As humans, we rely on the ability to walk in order to perform most daily functions – just think about a typical day in your life. Now, imagine you didn’t have a hip joint. Life would be a lot harder.
After the knee, the hip is the second largest weight-bearing, and one of the most important, joints in the body. It offers us the ability to walk, run, jump, dance, twirl…
The hip joint is a ball and socket synovial joint, joining the head of the femur (thigh bone) and the pelvic socket. Around these bones is a network of ligaments, cartilage and membranes, all of which helps the bones to glide past each other without any friction, damage or dislocation.
All of the components of the hip joint assist in the mobility. Damage to any part of the joint can have a massive effect on one’s mobility, range of motion and ability to bear any weight on the joint.
Orthopaedic degeneration or trauma can often result in a full or partial hip arthroplasty (replacements) or hip resurfacing.
Minimally invasive anterior hip surgery
A minimally invasive anterior hip surgery is similar to a hip arthroplasty, but with less cutting of the tissue around the hip joint.
Specially designed surgical tools are used in order to insert the artificial joints, and only one or small minor incisions are made. The incisions are so small, they allow for almost no tissue disturbance. This procedure leaves the gluteal muscles – the most important muscles for hip function – undisturbed.
THE KNEE
Crucial to daily life, the knee is the link between the femur (thigh bone) and tibia (shin bone). It’s a modified hinge joint comprising three components: the patella (kneecap), the patellar groove on the femur, and the medial and lateral tibiofemoral articulations linking the femur to the tibia. To support and add stability, there is a matrix of tendons and ligaments connecting the bones to the leg muscles. The knee, being a modified hinge joint, allows for flexion, extension, and slight internal and external rotation.
At birth, the patella is only cartilage. Between the ages of three and five years old, this cartilage patella ossifies and turns into bone.
The knee joint is vulnerable to injury and osteoarthritis. Osteoarthritis is the most common form of arthritis, caused by ageing and wear and tear of the cartilage. Other common knee injuries include patellofemoral syndrome (aggravation to the cartilage on the underside of the patella), patellar subluxation (the patella slides out of place or dislocates during activity) and patellar tendonitis (tendon inflammation).
TRAUMA
Trauma is accidental or intentional injuries that lead to life threatening situations. Trauma and orthopaedics is an area of surgery concerned with injuries and conditions that affect the musculoskeletal system (the bones, joints, ligaments, tendons, muscles and nerves).
SPORT INJURIES
Sports injuries result from acute trauma or repetitive stress associated with athletic activities. Sports injuries can affect bones or soft tissue (ligaments, muscles, tendons).
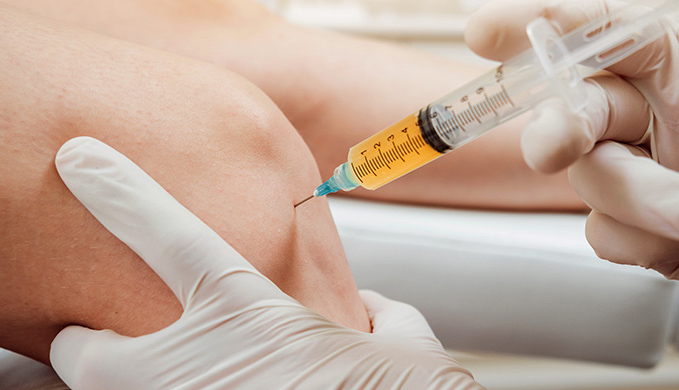
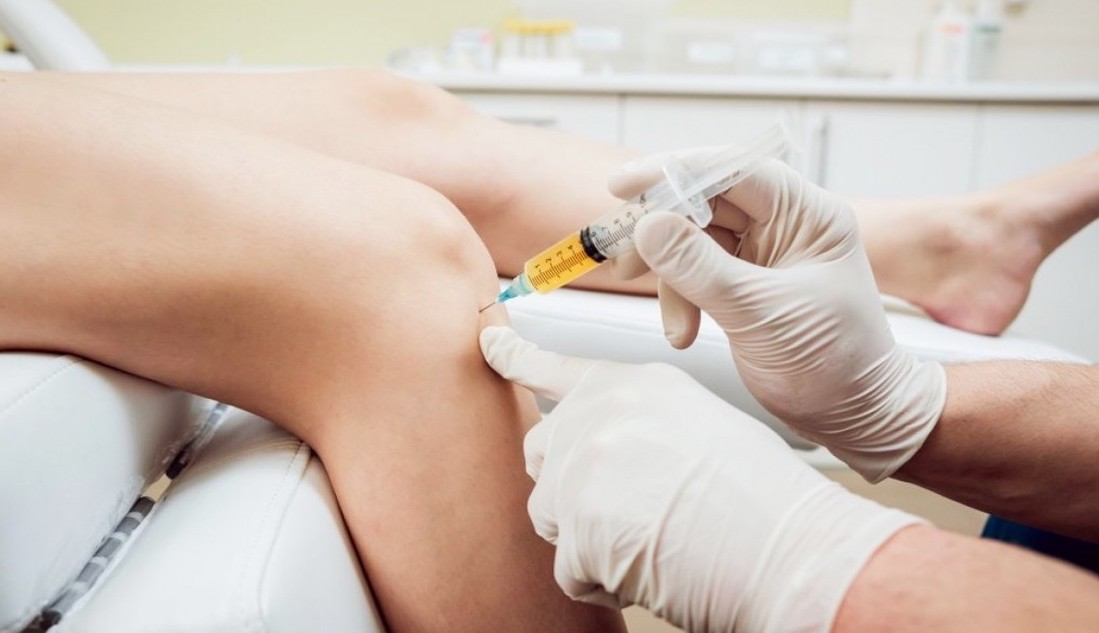
PLATELET-RICH PLASMA (PRP) THERAPY
Platelet-Rich Plasma (PRP) therapy is a state-of-the-art treatment that has been gaining popularity in orthopaedic medicine. It’s most commonly used to treat orthopaedic and sports injuries. PRP therapy is a form of regenerative medicine. Regenerative medicine centers on using the patient’s own body tissue, such as blood, fat, or bone marrow, to heal the body. When the body is injured, its natural response is to send platelets to the injury to begin the healing process. These platelets contain growth factors that are the main healing component in platelets.
Depending on the severity of the injury, it can take anywhere from weeks to months to heal on its own. In many cases individuals can suffer from chronic pain due to the injury for many years after the fact.
HOW DOES IT WORK
PRP therapy specifically utilizes high concentrations of the patient’s blood platelets to accelerate the healing process of an injury. PRP Therapy for orthopaedic conditions is administered via injection to the patient to begin the treatment process. These injections are designed to provide pain relief, reduce inflammation, and shorten recovery time.
PRP THERAPY AS AN ALTERNATIVE
There are several ways PRP therapy for orthopaedic conditions can be utilized. From soft tissue tears to inflammatory conditions like tendonitis, many patients are finding this treatment to be effective. Some patients are also unable to undergo surgery or have a sensitivity to anti-inflammatory medication. Patients now have another avenue for reducing or eliminating pain with PRP therapy for orthopaedic conditions.
At Atlantic Hip and Knee, our goal is to continue our education on new treatments so we may always offer effective solutions for our patients. We understand that there is not a one-size-fits-all answer for healthcare. We continue to dedicate ourselves to providing the best care for our patients. If you are interested in how PRP therapy or other treatment options for orthopaedic and sports injuries could benefit you, please schedule an appointment with us today.
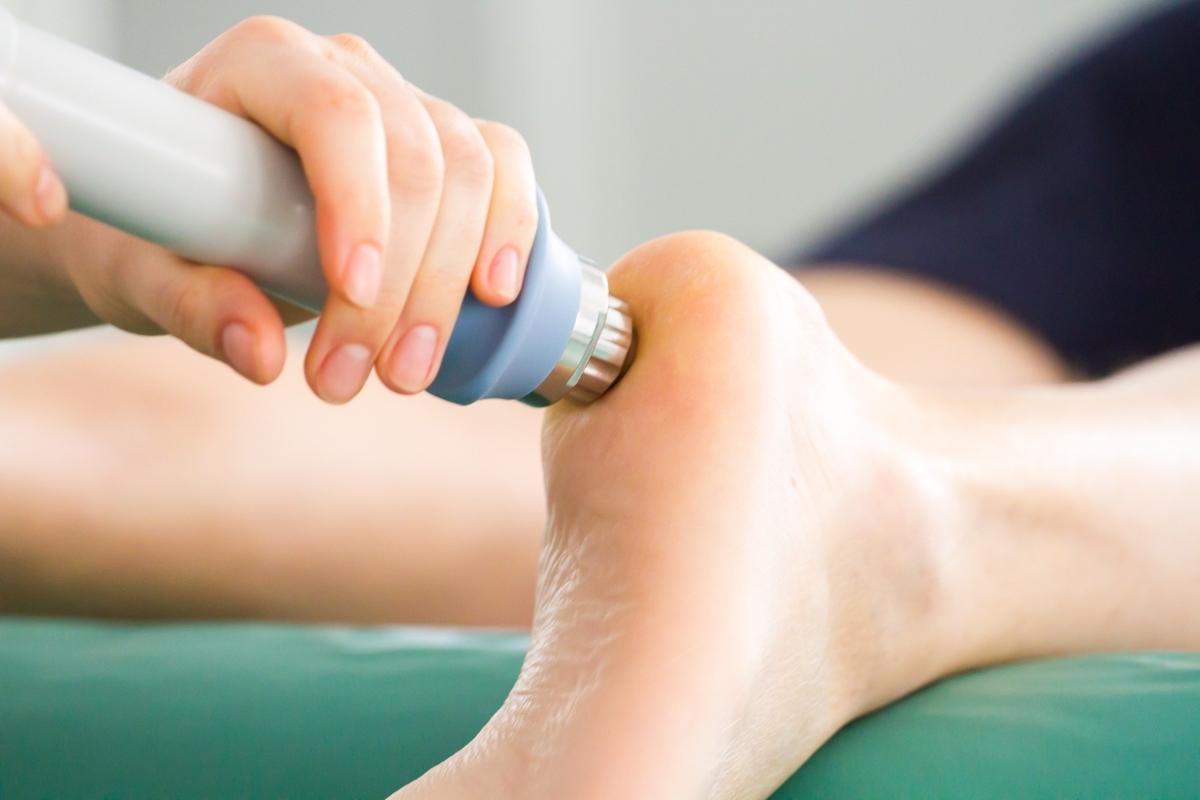
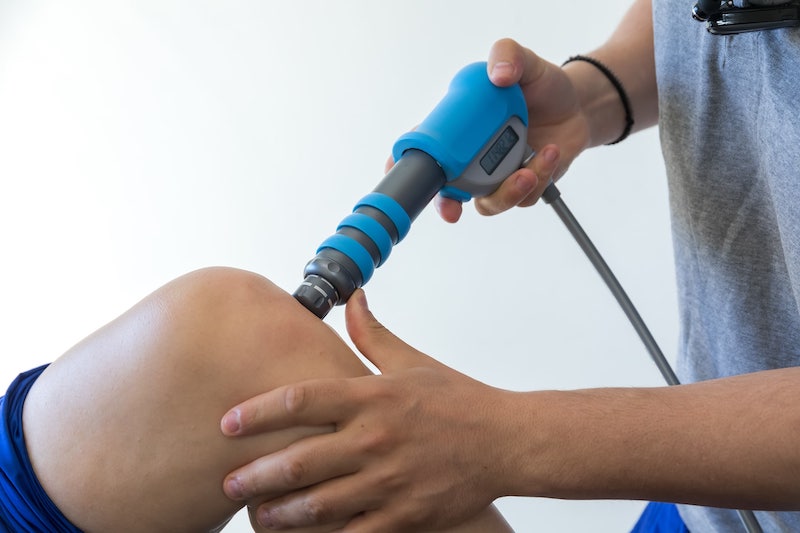
SHOCKWAVE THERAPY
Shockwave therapy is an innovative treatment aimed at healing chronic musculoskeletal conditions by purposely damaging the affected tissue. Musculoskeletal conditions include injuries or diseases that affect your muscles, ligaments, tendons, cartilage, and bones.
Also referred to as extracorporeal shockwave therapy (ESWT) and extracorporeal pulse activation therapy, shockwave therapy is a noninvasive treatment that uses high-energy ultrasound energy and mechanical waves to get the desired effects. When applied directly to your damaged tissue, the energy creates a type of injury, which stimulates your body’s natural healing powers to regenerate healthy tissue that replaces the damaged tissue.
Shockwave therapy was inspired by lithotripsy, which is a form of shockwave therapy urologists use to break up kidney stones. Urologists found that lithotripsy seemed to offer additional health benefits beyond breaking up kidney stones, including increased bone density and tissue regeneration. Researchers began to study the use of this medical technology for other treatments, including shockwave therapy for hard-to-treat, chronic musculoskeletal conditions.
THE REGENERATIVE POWER OF SHOCKWAVE ENERGY
At Atlantic Hip and Knee, Dr Mark van der Kaag seeks out treatments that support your body’s natural healing power to repair damaged or injured tissue, reduce pain, and restore mobility so that you don’t need invasive procedures.
The exact mechanism of how shockwave therapy works isn’t fully understood. However, according to a March 2012 report published in the Journal of Orthopaedic Surgery and Research, researchers theorize that the energy produced by the innovative tool triggers a microscopic response in the cells of the damaged tissue — purposely damaging the tissue — that stimulates regeneration of new, healthy tissue.
WHO BENEFITS FROM SHOCKWAVE THERAPY?
Dr van der Kaag uses shockwave therapy to treat many chronic musculoskeletal conditions, as well as acute sports injuries. You may benefit from the treatment if you suffer from:
- Golfer’s elbow
- Tennis below
- Rotator cuff tendinitis
- Plantar fasciitis
- Achilles tendon
- Chronic hamstring pain
- Quad/patellar tendinitis
- Frozen shoulder
- Gluteus medius/lateral hip tendon (also known as greater trochanteric bursitis or hip bursitis)
- Stress fractures
- Athletes with acute muscle and tendon injuries, such as those that affect the hamstring or groin, also benefit from shockwave therapy.
TREATMENT
It’s not uncommon to experience pain during your shockwave therapy, but the actual treatment only takes a few minutes. You can expect a gradual improvement in pain and mobility in the treatment area within a few days of starting treatment, with continued improvement over the next several months.
Depending on the severity of your musculoskeletal issue, you may benefit from a series of 3-5 treatments at weekly intervals to get the best possible results. For athletes, Dr van der Kaag may perform daily shockwave therapy to accelerate healing and help the athlete get back to their sport faster.
Don’t let your injury or chronic pain condition prevent you from living a full life. With innovative shockwave therapy, relief is possible. This treatment is available at Mediclinic Panorama. Please get in touch today to learn more.